Patient Air Transfer Guide: From Pre-Assessment To Safe Handover
Patient Air Transfer is not only a flight—it is a carefully managed medical process that starts long before takeoff and ends only after a safe handover at the receiving hospital. At TKP Medical Assistance, we design each transfer as a step-by-step pathway for the patient and the family: clear decisions, stable clinical care, and smooth coordination across borders.

1) What a Patient Air Transfer Really Includes
Many families imagine “air ambulance” as a single service. In reality, a Patient Air Transfer is a chain of clinical and operational actions. If one link is weak, the whole journey becomes stressful. A strong provider builds a complete pathway that covers medical assessment, flight planning, ground logistics, and hospital coordination.
From our frontline work, families usually need three things most: safety, predictability, and dignity. That is why TKP operates as a direct provider, not an intermediary. We plan, coordinate, and deliver the mission with our own medical and operations teams. This reduces communication gaps, shortens decision cycles, and keeps accountability clear—especially when time matters.
With over 24 years of experience and more than 10,000 successful missions, TKP has built practical systems around real-world urgency. Those systems help families avoid common risks such as delayed approvals, unclear responsibilities, or fragmented updates during a long-distance transfer.
2) Pre-Assessment: Turning Medical Uncertainty Into a Clear Plan
A safe Patient Air Transfer begins with a clinical pre-assessment. This is the moment where confusion can become clarity. Your provider should explain what the patient needs during transport, what risks must be controlled, and what level of medical team and equipment is required.
At TKP, experienced ICU-led teams review the patient condition and define the transport level. This is not “paperwork.” It directly guides key choices such as oxygen strategy, monitoring requirements, airway support, and whether advanced systems like ECMO might be needed.
A practical pre-assessment should give families understandable answers:
• What must remain stable during transfer (vitals, oxygenation, airway, circulation)
• What could worsen in flight and how it will be prevented
• What equipment and staffing level will be used for this case
• What timeline is realistic based on medical readiness and approvals
When these points are made clear early, families can make confident decisions instead of guessing under pressure.
3) In-Flight ICU Capability: Why Equipment and Certification Matter
A Patient Air Transfer should feel like “ICU-level continuity,” not a risky gap between two hospitals. That is why clinical capability in the air is not a marketing phrase—it is a real safety layer.
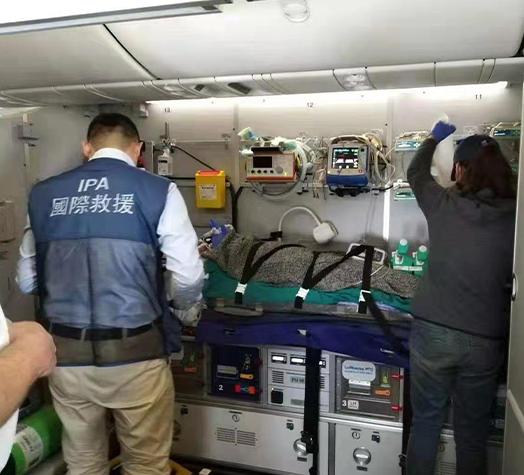
Every TKP mission is equipped with portable advanced life support systems and transport-ready ICU tools. Depending on the case, this may include ICU monitors, oxygen supply, ventilators, and ECMO when required. Importantly, the equipment is aviation-certified and configured for both adult and pediatric patients. This matters because aviation conditions demand stable power, secure mounting, and reliable performance under vibration and altitude changes.
Team qualification matters just as much as machines. TKP teams are ACLS & BLS certified, which means they are trained for advanced and basic life support scenarios. For families, the value is simple: if the patient’s condition changes mid-journey, the team is prepared to respond immediately, not “wait until landing.”
In practice, strong clinical readiness reduces avoidable emergencies, helps keep vital signs stable, and supports a calmer experience for the family.
4) 24/7 Coordination: How Good Operations Protect the Patient
A Patient Air Transfer is a medical mission, but it is also a logistics mission. Delays can increase risk, and miscommunication can create real harm. That is why operations quality is a form of patient protection.
TKP runs 24/7/365 global coordination with multilingual staff (EN/CH/CN). This is designed for real cross-border complexity, where families may be in one country, the patient in another, and the receiving hospital somewhere else again. A round-the-clock team reduces waiting time and prevents “handoff gaps” between time zones.
A reliable coordination center typically manages:
• Dynamic scheduling based on urgency and patient condition
• Flight permissions, airport selection, and ground ambulance matching
• Coordination with hospitals, insurers, and relevant institutions
• Real-time journey tracking and family updates
For families, real-time updates are not a luxury. They reduce anxiety, help with hospital arrival planning, and prevent the feeling of being “left in the dark” during critical hours.
5) Route Planning: Reaching the Right Hospital Faster and More Smoothly
Families often ask, “Can you reach our location?” The better question is: “Can you reach safely and efficiently, even if the location is difficult?” Not all airports have the same infrastructure. Not all routes are equal in speed and stability. A professional Patient Air Transfer provider must plan routes with both safety and access in mind.
TKP’s route planning is built for flexibility. We can use strategically selected airports, including those with limited infrastructure, to connect patients from remote or underserved areas to leading medical facilities. This is especially important for regions where the nearest major airport is not close to the patient.
Good route planning focuses on practical outcomes:
• Reducing total transfer time (not only flight time)
• Maintaining clinical stability (less unnecessary movement)
• Avoiding predictable delays (permits, ground access issues, unsuitable airports)
• Keeping the receiving hospital prepared for immediate admission
When routes are planned with medical logic first, the patient arrives in better condition—and the receiving team can act faster.
6) Safe Handover: The Final Step That Completes the Transfer
A Patient Air Transfer is not complete when the aircraft lands. The final step is the safe handover: the moment clinical responsibility transfers to the receiving hospital team. This stage must be structured, documented, and calm.
At TKP, the process is designed to keep care continuous from pre-assessment to final handover, with monitoring and specialized support throughout the journey. Families benefit from a smoother landing-to-bedside transition, fewer surprises at admission, and clearer communication with the receiving clinicians.
A structured handover delivers decision-ready information: a concise clinical brief, transport monitoring trends, medications administered, interventions performed, and a clear account of key events during transfer. This helps the receiving team act immediately and prevents treatment delays linked to incomplete records.
• CTA (Call-to-Action):
If your family is arranging a Patient Air Transfer—domestic or international—contact TKP Medical Assistance with the diagnosis, hospital location, and urgency level for a coordinated plan. Our ICU-led team will complete a practical pre-assessment, recommend the right transport configuration, and provide a clear coordination plan designed for a safe, dignified handover.
Submit Your Request
Recent Posts
Tags
- Air Ambulance
- Bedside To Bedside
- Cross Border Aid
- Emergency Evacuation
- Global Medical Rescue
- How can I ensure the patient's stability while in the air?
- How do I request an air medical transport?
- How is it different from an air ambulance
- how to activate emergency aircraft service
- how to request an air ambulance
- Is air medical transport safe
- Is international transport possible
- Medical Rescue
- Medical Transport
- Patient Repatriation
- Remote Rescue
- Seamless Coordination
- Telemedicine Support
- Tourists And Expats Medical Escort
- What are the benefits of a cross-border medical transfer
- What are the different types of transfers
- What are typical use cases
- What documents do I need to prepare for a transfer?
- What does high-speed rail patient transfer stands for
- What is air ambulance
- What is air medical transport?
- What is cross-border medical transfer
- What is emergency aircraft
- what is high-speed rail patient transfer
- What is medical charter flight
- what is neonatal ICU transfer
- What is patient air transfer
- What medical equipment is available on board the aircraft
- What situations shouldn't use air medical transport?
- What types of air ambulance are there?
- What types of air ambulance exist
- What's the difference between international and domestic transfers?
- what’s the difference between air medical transport and regular ambulance?
- When is emergency air transport necessary
- Which patients require air medical transport?
- who is included in the medical team
- who needs an air ambulance






